Bunion / Hallux Valgus
What is a bunion?
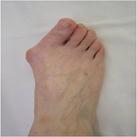
A bunion / Hallux Valgus is term for a boney bump that has formed on the inner aspect of the forefoot at the main big toe joint (Fig 1).
The medical term is hallux valgus, hallux being the latin name for the big toe, valgus describing the leaning of the big toe away from the midline of the body. This condition can run in families, presenting as early as adolescence or be acquired in later life (eg. as a result of footwear).
What are the symptoms of a bunion and how is it diagnosed?
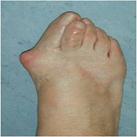
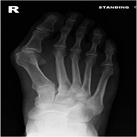
Symptoms include pain in the bump area with or without shoes and occasionally associated discomfort in the ball of the foot (metatarsalgia) and/or lesser toe deformities (Fig 2) such as a hammertoe from direct pressure of the big toe. The diagnosis is confirmed by clinical assessment and x-rays (Fig 3).
How is a bunion treated?
Treatment primarily includes shoe modification (ie avoiding uncomfortably tight shoes) or pads and special bunion splints that are commercially available on the high street.
When is bunion surgery necessary?
Bunion surgery is indicated when symptoms are significantly troublesome, have been present for some time (eg >months) and have not responded to simple non-operative measures. Cosmetic considerations alone are not a good indication for surgery.
What does bunion surgery involve?
Bunion surgery aims to narrow the often widened forefoot and, thus eliminate or reduce the inner bump. As a result the big toe is straightened and no longer pushes across the lesser toes. The weight-bearing forces are, thus, redistributed, the big toe becomes more functional again and any pain in the ball of the foot (metatarsalgia) may also subside.
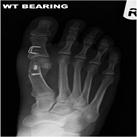
Several surgical techniques are available and Mr Weitzel will advise the patient of the most appropriate for her/his individual problem. This will often include a form of osteotomy (cutting and realigning of bone Fig 4) which is then fixed with internal implants such as screws and/or staples.
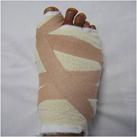
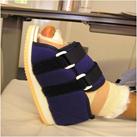
Bunion surgery is carried out as a day case procedure under general, spinal or regional anaesthesia. A regional ankle block (with local anaesthetic) is routinely used for postoperative pain relief (usually lasting 6-8hours). Postoperatively a soft bandage protects the foot (Fig 5) and mobilisation is through a solid-soled postoperative shoe (Fig 6).
Click here for Bunion Surgery Information Video by Bupa
What happens after bunion surgery?
Follow-up appointments are made at around 2 weeks (for wound check) and 6 weeks (Xray check) after the operation. Depending on the patient’s occupation and commute requirements return to work can be within 1-2 weeks (office-type work) or take much longer ie 4-8 weeks (physical labour). Full recovery eg until return to all physical activities such as sports and until all types of footwear can be worn may take 2-3 months.
What is the outcome of bunion surgery?
Generally, the outcome of bunion surgery depends on several factors including the severity of the clinical deformity and pre-existing joint wear, the avoidance of complications as well as the patient’s ability to follow the postoperative instructions closely. Overall, 90-95 % of patients are satisfied with the result.
Minimally Invasive Surgery (MIS)
In the recent past minimally invasive bunion surgery has been gaining popularity in the UK. Mr Weitzel is one of the first surgeons in the southeast and London area trained in MIS technique and has been treating a number of patients by this method. This involves performing the same surgery via a number of small incisions rather than one or two longer incisions and using a special burr under X-ray guidance.
In his opinion at present the only advantage compared to open surgery lies in the better cosmetic appearance of the skin postoperatively. The results in terms of postoperative pain, speed of recovery, return to activities/work and general outcome appear comparable to open surgery. Clinical evaluation of MIS surgery is ongoing and in the not too distant future the type of patient best to benefit from MIS is likely to become apparent.
Bunion related images
Click on image to enlarge